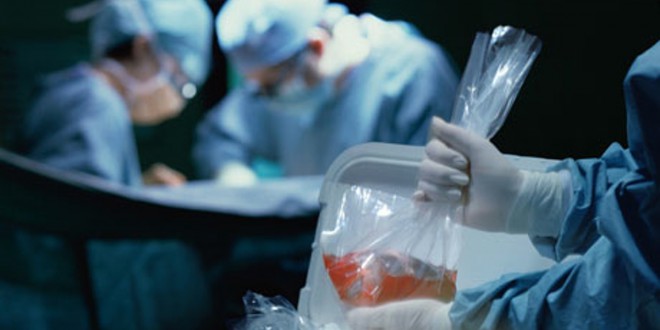
Should social support be an eligibility criterion for organ transplantation?
Current guidelines state that doctors should consider the “social support” of patients.
While medical factors are part of the eligibility assessment for organ transplantation candidates in the United States, “social” considerations are also taken into account when evaluating patients.
Current guidelines from the Centers for Medicare and Medicaid Policy (CMS) and professional societies state that doctors should consider the “social support” of patients when assessing their eligibility for organ transplantation. The definition of “social support” is notoriously vague, but it is typically taken to refer to the presence of family and friends who can assist a patient in keeping to their postoperative treatment and recovery plan.
Yet two new studies published by researchers from Tufts University criticise the inclusion of the criteria in eligibility guidelines, saying that it disproportionately affects people of color, people on low incomes, and those living in rural areas.
Researchers surveyed almost 600 transplant clinicians about various criteria they use in deciding if a patient qualifies for a kidney transplant. Results indicated that “social support” was the second most important factor in listing decisions for both psychosocial evaluators and medical and surgical providers. This was surprising, considering that one in four of respondents thought the criterion was an unfair standard.
The authors of the studies questioned the ethical acceptability of the standard. “In other areas of health care, we do not exclude patients from life-saving treatment merely because they do not have friends or family available,” said Kerin Ladin, assistant professor in the department of Occupational Therapy at Tufts and a lead author on the studies.
In one of the studies, published in the Journal of Medical Ethics, the authors write:
Persons of low socioeconomic status, racial and ethnic minorities, and those living in rural areas face disproportionate difficulty successfully completing transplant evaluations. Because demonstrating social support may be correlated with socioeconomic status, race, ethnicity and age, this criterion may increase and reinforce barriers to care for underserved populations.
Should social support be an eligibility criterion for organ transplantation?
Xavier Symons
Creative commons
https://www.bioedge.org/images/2008images/organ_on_ice.jpg
egalitarianism
inequality
organ transplantation
us
